Authors Jesse K. Placone, Bhushan Mahadik, and John P. Fisher explore the benefits and challenges of tissue engineering. In the recently published ‘Addressing present pitfalls in 3D printing for tissue engineering to enhance future potential,’ the authors also address the future potential for 3D printing, and accompanying materials and techniques.
Noting that bioprinting is intrinsically limited due to the difficulty in sustaining human tissue, the authors explore how obstacles can be overcome, as well as the potential for use in ‘academic, clinical, and commercial settings.’ Many researchers today are also focused on tissue engineering for cells to be used both in vitro and in vivo. Due to challenges with size, nutrients for cells, and waste diffusion, many studies today are centered around creating microvasculature.
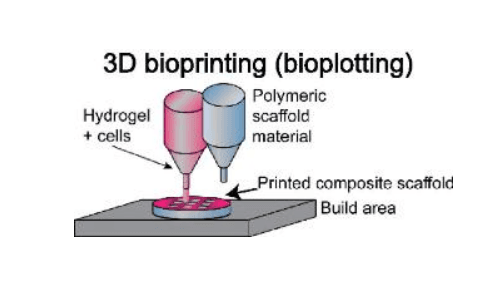
Popular materials for use in bioprinting are polycaprolactone (PCL), poly(lactic-co-glycolic acid) (PLGA), and polystyrene (PS), along with a variety of bioinks, and a range of techniques.
“Particularly, there is a high degree of freedom when 3D printing acellular, single-material constructs with either hydrogels or thermoplastics,” state the authors.
The Role of 3D Printing in Medicine
The use of multi-material printing with hybrid bioinks is becoming increasingly popular too, allowing for successful fabrication of bone mimetics, for example, creating rigid support materials as well as softer ones for ‘the desired cellular response.’ While a wide range of research studies have been and are in the process of being performed around the world, there has been particular attention paid to the musculoskeletal system, along with forays into fabrication of cartilage, tendons, skin, applications for wound care, and more.
“Current clinical treatments for skin regeneration focus mainly on the epidermal layer and are unable to capture the intricate neurovascular, follicular, and sebaceous gland architecture of the dermal and hypodermal layer,” state the authors. “Consequently, 3D printing research has aggressively focused on recreating these distinct, yet interconnected layers in order to provide more meaningful clinical treatments and therapies for patients suffering from severe 2nd and 3rd-degree injuries.”
Biocompatible Materials and Processes
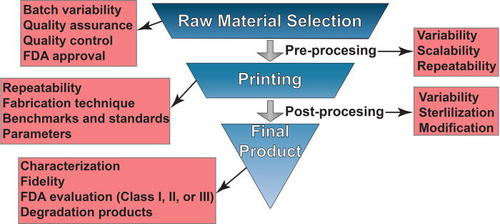
Key steps to generate clinically relevant 3D printed substrates. At each development and fabrication step, researchers need to aid in the development of standards as well as evaluation and characterization methods to ensure repeatability. Consideration needs to be taken with the scale up of each of these steps when transitioning from small scale laboratory settings to larger scale fabrication approaches. Additionally, hands on training and formal education regarding the different parameters that need to be controlled as well as the limitations and constraints on different fabrication strategies will be critical for the continuous adoption of this technology as it matures.
The ability to customize nearly any product is one of the greatest benefits to 3D printing, and it translates significantly to the bioprinting realm in allowing for implantation of a patient’s own cells—offering the most patient-specific care possible, and especially in terms of the future for organ transplants.
3D printing is offering tremendous impacts in regenerative medicine too, with possibilities for every organ. Again, while there are inherent challenges when dealing with cells, with time and effort expended toward the study of and sustainability of tissue in the lab, complex structures can be fabricated.
“Researchers should place an emphasis on guiding the field toward developing standard techniques and aid in the adoption of standards of regulatory agencies to provide a framework for clinical translation,” concluded the researchers. See also: The Complete 3D Printing Filament Guide: Types, Pr…. “Establishing centers of 3D printing excellence would facilitate the transition from the bench to clinical applications by localizing the expertise and minimizing the logistical problems that may plague individual groups.”
Clinical Applications and Case Studies
“As the field continues to mature, addressing these barriers will enable the transition of 3D printing from niche applications to a more widespread technique for 3D culture, high-throughput screening, and device and implant fabrication.”
What do you think of this news? Let us know your thoughts! Join the discussion of this and other 3D printing topics at 3DPrintBoard.com.
[Source / Images: ‘Addressing present pitfalls in 3D printing for tissue engineering to enhance future potential’]
The post Researchers Address Benefits and Pitfalls in 3D Printing of Tissue appeared first on 3DPrint.com | The Voice of 3D Printing / Additive Manufacturing.
Regulatory Considerations and Safety
from Your daily news from 3DPrint.com http://bit.ly/33dgdba
Related Articles
Frequently Asked Questions
How is 3D printing used in medicine?
3D printing is used in medicine for surgical planning models, custom implants, bioprinting tissue scaffolds, drug delivery systems, dental aligners, and prosthetics. It enables patient-specific solutions that improve outcomes and reduce surgery time.
What materials are biocompatible for 3D printing?
Common biocompatible materials include PEEK, titanium alloys (Ti6Al4V), bio-ceramics (hydroxyapatite), medical-grade resins, PLA for temporary implants, and hydrogels for bioprinting. Material choice depends on the application and required mechanical properties.
Is 3D printed medical equipment FDA approved?
Yes, several 3D printed medical devices have FDA clearance, including orthopedic implants, dental restorations, and surgical guides. Each device must go through the appropriate regulatory pathway based on its risk classification.
📌 Related Articles
- The Current State of Metal 3D Printing in 2020
- The Complete 3D Printing Filament Guide: Types, Properties & When to Use Each
- 3D Printing News: Multi-Material Breakthrough and Aerospace Market Boom
- ABS 3D Printing Settings Guide: Temperature, Enclosure, and Cooling for Strong Parts
- Best Budget 3D Printer Upgrades That Actually Improve Print Quality: Belts, Springs, Hotends & More