Finnish researchers report on inaccuracies in the AM process chain, releasing their findings in ‘Cumulative Inaccuracies in Implementation of Additive Manufacturing Through Medical Imaging, 3D Thresholding, and 3D Modeling: A Case Study for an End-Use Implant.’
3D printing emerged in the 80s as a prototyping tool, but over the years designers and engineers have begun to rely on the technology for functional and critical parts in applications like automotive/racing and aerospace; however, the medical realm has been enormously—and positively—impacted with greater access to 3D printed models, devices, and implants.
“AM has been widely implemented in the medical industry, and it has gained clearance for more than 80 AM medical devices such as maxillofacial implants and a knee joint replacement system from the United States Food and Drug Administration (FDA),” state the authors in their study.
The Role of 3D Printing in Medicine
“Substantial AM growth is enabled by its economical lot-size-one that allows for unprecedented geometrical freedom in one build cycle using minimal set-up because it is a general-purpose digital technology which is not constrained by patient-specific tooling. Further, it enables a unique supply chain with increased communication and responsiveness that complements the state of urgency in the medical field.”
Customized implants are often made from titanium today, especially for those targeting the head or neck area. Still, there is greater need for porous titanium, able to promote osseointegration with the correct mechanical properties in place. There is also greater need for error-free imaging, leading to better patient-specific treatment as CT scans are converted to 3D images and consequently, 3D prints. While fan-beam multi-slice CTs (MSCT) are used, and may offer better resolution in terms of low contrast, the cone-beam CT (CBCT) system offers the following benefits:
- Acceptable image quality
- Good scanning time
- Better affordability
- Reduced radiation dose
As 2D images are converted to 3D, however, the use of thresholding techniques is required, whether users employ a volume-based, contour-based, or point-cloud-based approach. Volume-based is most commonly used, via a marching cubes algorithm.
“Each step of the process can contribute geometric error to the resulting implant,” stated the researchers.
Biocompatible Materials and Processes
Over time, researchers have studied the chain of inaccuracies in CT systems and resulting processes, resulting in questions regarding details like voltage, thresholding values, software, varying AM techniques, varying hardware, and more, leaving the authors here to note that all of these concerns ‘have prompted additional verification studies that account for the whole process chain.’
In following a case study involving pre-operative planning for an implant, the authors investigate possible inaccuracies and how they impact an end-use implant.
Clinical Applications and Case Studies
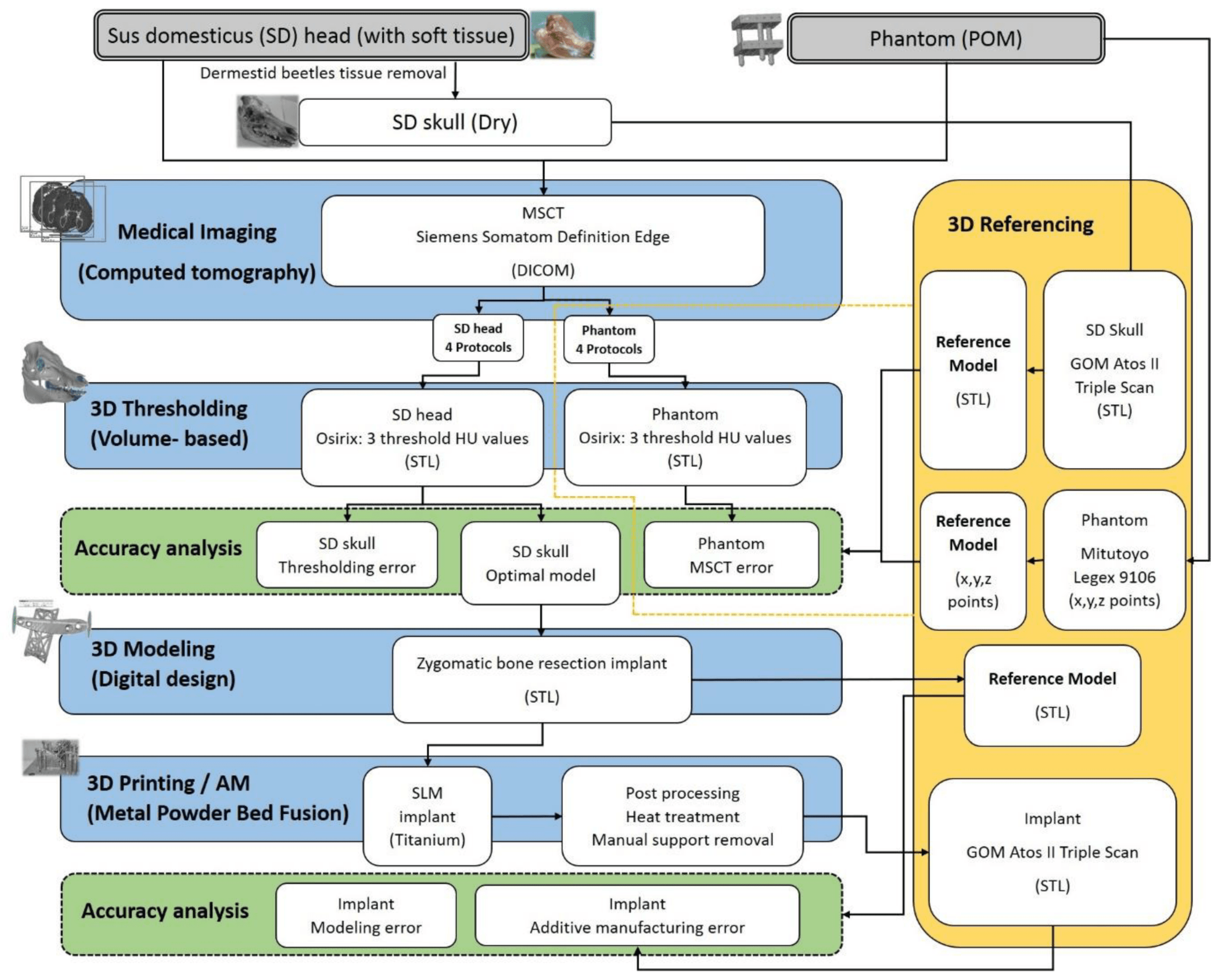
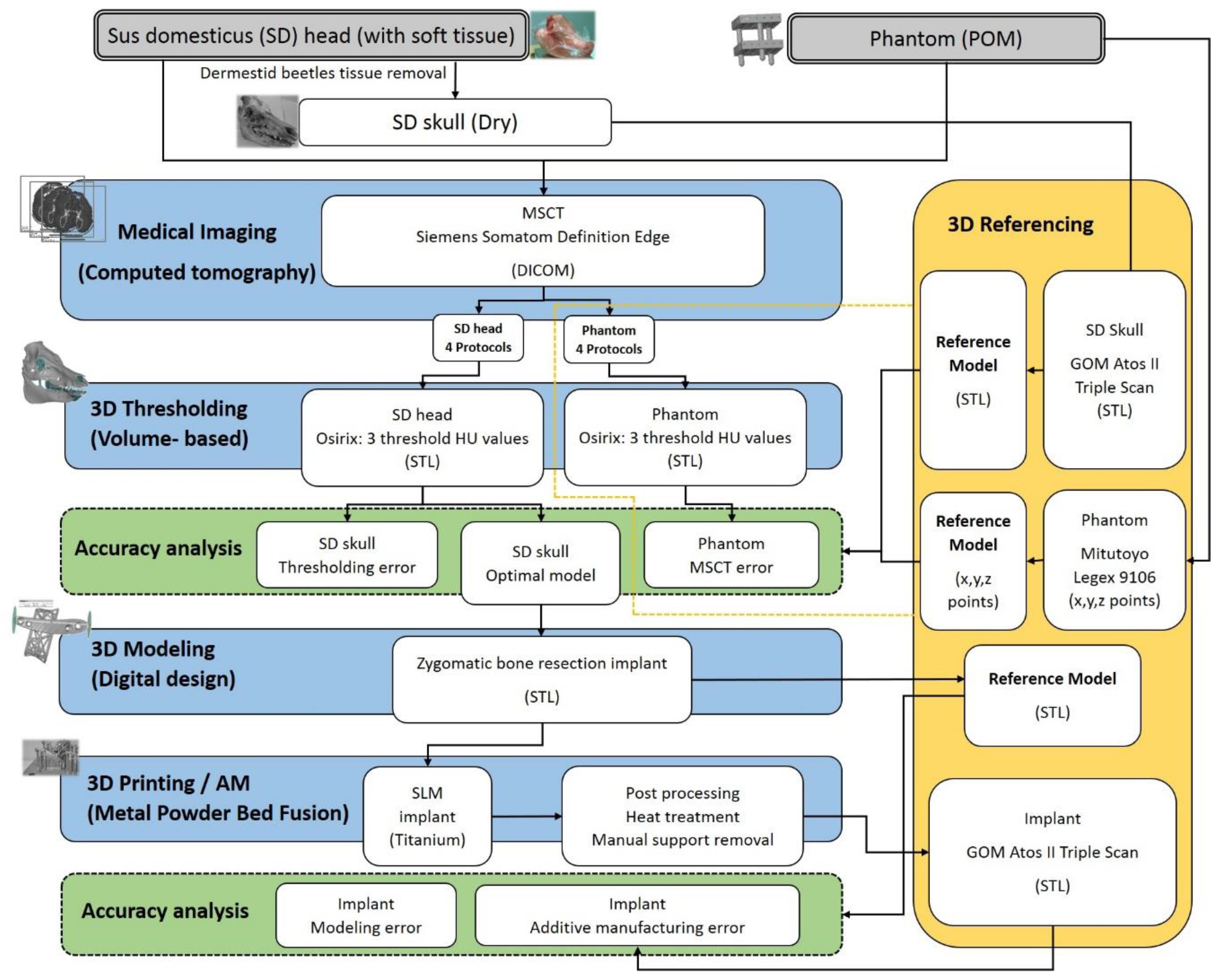
The process of evaluating cumulative inaccuracies for an end-use implant.
Using a nine-month old dry skull from a pig, the researchers scanned the specimen and made reference points. They also designed a QA phantom for confirming measurements, made of Polyoxymethylene (POM), a material used for several QA phantoms in other studies.

Regulatory Considerations and Safety
The quality assurance Phantom for examining the MSCT imaging error.
“Assuming a case where a patient had to undergo a resection of a zygomatic bone tumor, an implant was digitally modeled to replace the deformity using 3Data Expert (11.0.0.32, Deskartes Oy, Espoo, Finland) software. The implant was designed using the right zygomatic bone projections of the SD head that were obtained from the optimal CT imaging and thresholding parameters,” stated the researchers.
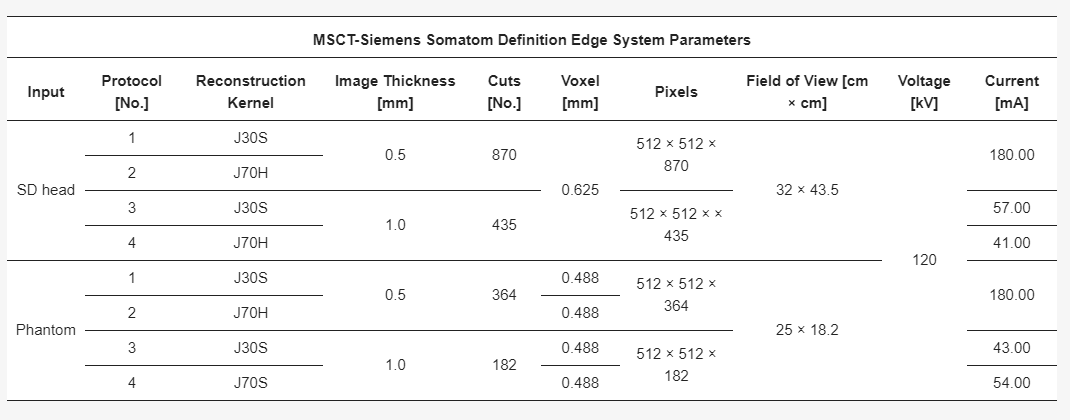
Parameters of multi-slice computed tomography (MSCT) imaging for the sus domesticus (SD) head and the Phantom.
Research Breakthroughs and Innovations

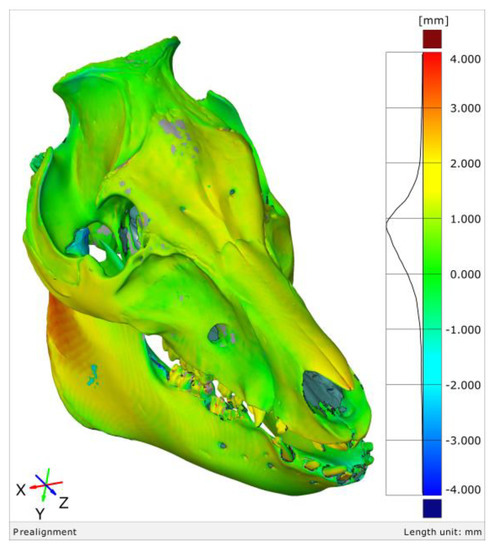
The mesh sensitivity analysis of the SD skull surface with respect to the segmented SD head surface.
“The worst-case CT imaging error emerged in the z-axis of the MSCT system and generated the second least error value compared to the other processes,” stated the researchers.
Results showed that the surface did contain a suitable mesh size, at ‘steady state values’ from the third to the sixth iterations. The thresholding error for this case showed negatively skewed asymmetric deviations to the left. The authors noted that this error was ‘one of the most significant errors compared to the other processes,’ leading them to recommend that medical professionals should be aware that the error ‘enables correction of a systematic effect for the implant.’
The Future of Bioprinting and Medical AM
Such an error also propagates to the implant as it was created as a negative of the segmented sample head. See also: 3D Printing Safety Equipment Guide: Respirators, G…. Manual thresholding alternatives may be required too, and while that may take extra time, the authors suggest that such effort may yield more accurate .stl models.
The Role of 3D Printing in Medicine
The thresholding error of the segmented SD head on the dry skull with the verified mesh size.
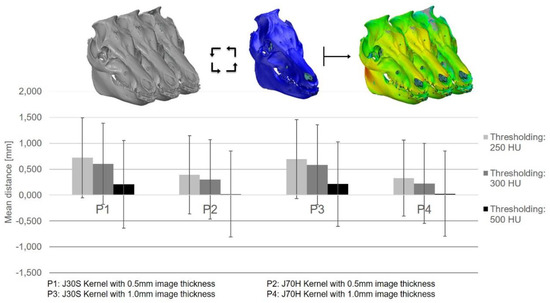
The thresholding error of the segmented SD head as a function of the CT Protocols and Hounsfield units with respect to the optically scanned dry skull (blue).
“Practitioners that require a high accuracy for the implants, e.g., the orbital floor implants, should respect the recommended safety margin. The prescribed correction measures can be taken if the intended processes and equipment are identical to this study or after implementing the applied methodology with the relevant processes and equipment as a quality control and assurance protocol,” concluded the researchers.
Biocompatible Materials and Processes
“Moreover, it should be considered that it may not always be absolutely imperative to design the implant to fit perfectly at the initial phase. The perforation of the lingual mucosa is one of the complications related to the patient-specific implant. If the lingual foil of the implant scaffold is too high, it is prone to perforate the lingual mucosa during the postoperative healing. For example, the extraction of teeth in the osteotomy line will lead to a resorption and further, remodeling of the marginal alveolar crest, which has to be considered during the planning of the implant.”
What do you think of this news? Let us know your thoughts! Join the discussion of this and other 3D printing topics at 3DPrintBoard.com
[Source / Images: ‘Cumulative Inaccuracies in Implementation of Additive Manufacturing Through Medical Imaging, 3D Thresholding, and 3D Modeling: A Case Study for an End-Use Implant’]
The post Finland: Studying the Impact of Medical Imaging Inaccuracies on End-Use Implants appeared first on 3DPrint.com | The Voice of 3D Printing / Additive Manufacturing.
Related Articles
Frequently Asked Questions
How is 3D printing used in medicine?
3D printing is used in medicine for surgical planning models, custom implants, bioprinting tissue scaffolds, drug delivery systems, dental aligners, and prosthetics. It enables patient-specific solutions that improve outcomes and reduce surgery time.
What materials are biocompatible for 3D printing?
Common biocompatible materials include PEEK, titanium alloys (Ti6Al4V), bio-ceramics (hydroxyapatite), medical-grade resins, PLA for temporary implants, and hydrogels for bioprinting. Material choice depends on the application and required mechanical properties.
Is 3D printed medical equipment FDA approved?
Yes, several 3D printed medical devices have FDA clearance, including orthopedic implants, dental restorations, and surgical guides. Each device must go through the appropriate regulatory pathway based on its risk classification.
📌 Related Articles
- The Current State of Metal 3D Printing in 2020
- 3D Printing Safety Equipment Guide: Respirators, Gloves, and Ventilation for 2026
- 3D Printing News: Multi-Material Breakthrough and Aerospace Market Boom
- 3D Printing Tungsten Carbide: How Hot-Wire Laser Technology Creates Metal Harder Than Steel
- ABS 3D Printing Settings Guide: Temperature, Enclosure, and Cooling for Strong Parts