Researchers from the US and China have been working together to improve treatment for erectile dysfunction (ED), releasing the details of their study in “Functional reconstruction of injured corpus cavernosa using 3D-printed hydrogel scaffolds seeded with HIF-1α-expressing stem cells.” Treatment for ED can be difficult, with a multitude of different therapies and medications prescribed worldwide; however, in this study, the researchers focused on treatment for men with actual injury to the erectile tissue, seeding heparin-coated, 3D-printed hydrogel scaffolds for furthering the development of bioengineered vascularized corpora.
Once damaged, the corpus cavernosum is not a candidate for regenerative treatment. And, while lack of erectile function is a major concern, urinary function can be affected, too, leading to even more serious problems. The authors report that, though transplantation may be an option, it is controversial. Accellular matrix replacement has been considered as a possibility also, but one that yields numerous challenges and some lack of success. In seeking a comprehensive solution, the researchers turned to 3D printing “complex biomimetic structures.”
“The hydrogel scaffold was selected because it could be developed to have a mechanically strong porous structure that provided a good microenvironment and space to support cell growth, adhesion and migration, and thus structurally and mechanically match the natural corpora cavernosa,” explained the researchers. “The reconstruction of the microvascular system plays a vital role in the recovery of corpora cavernosa functions.”
The Role of 3D Printing in Medicine
Because of the obvious and critical role that blood supply plays in successful treatment, the researchers fabricated scaffolds that could not only reduce fibrosis from the defect, but also restore the vascular network and necessary tissue. HIF-1α mutated muscle-derived stem cells (MDSCs) were seeded onto the scaffolds for implantation into the corpora cavernosa.
Biocompatible Materials and Processes
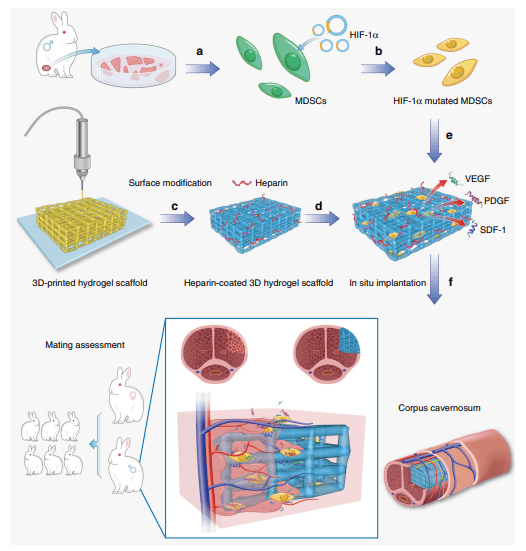
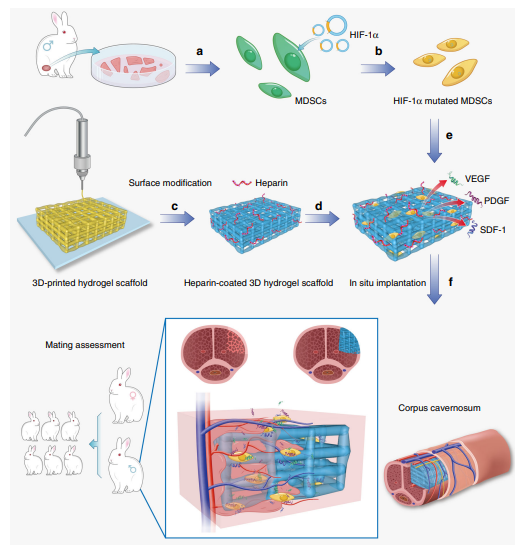
The schematic illustration of repairing injured corpora cavernosa in rabbits. a The MDSCs were extracted from muscles of rabbit legs. b The HIF1α-mutated MDSCs were obtained by lentiviral transfection. c 3D-printed hydrogel scaffold was prepared by 3D printing technology. d Heparin was deposited onto the surface of 3D-printed hydrogel scaffold by layer-by-layer self-assembly to obtain a heparin-coated hydrogel scaffold. e The HIF-1αmutated MDSCs were seeded on the heparin-coated hydrogel scaffold and secreted angiogenesis-related factors. f The scaffold was implanted in the rabbits with cavernosum injury to repair the penile corpora cavernosa in situ and restore penile erection and ejaculation function. Additionally, baby rabbits were born due to the recovery of the penile erection and ejaculation function (and the subsequent reproductive capability) of the male rabbits through our treatment. Our strategy can lead to the recovery of penis morphology and the reconstruction of the microvascular system in the penile corpora cavernosa.
The process was successful, with results seen within four months. The researchers noted that, post-harvest in mice, the scaffolds showed no tissue necrosis; were found to be degradable; and also sustained tissue viability in vivo. More new blood vessels were found in the heparin-coated scaffolds for the mHIF1α group than others, with new tissue growing over the whole scaffold, filling the pores during the degrading process. This led the researchers to note that overall data demonstrated that the mHIF-1α group “promoted the healing of the injured corpus cavernosa compared to the other implantation groups.”
Clinical Applications and Case Studies
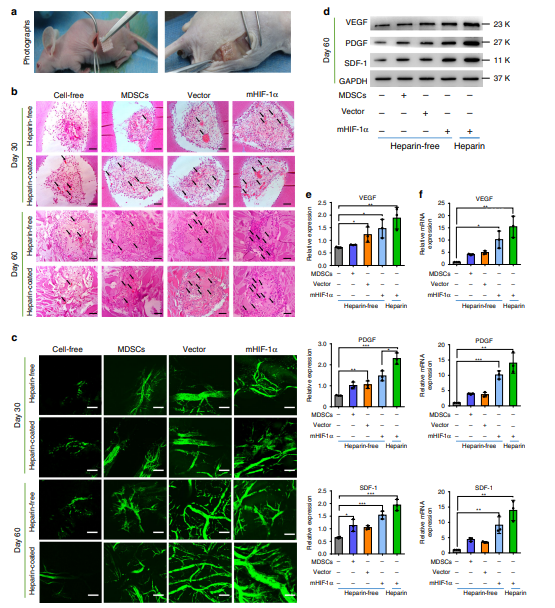
Experimental evaluation of subcutaneous implantation with cell-loaded 3D hydrogel scaffolds in nude mice. a Images of heparin-free and heparincoated 3D hydrogel scaffolds loaded with different cells before and 60 days after subcutaneous implantation. b Images of H&E staining in the cell-free, MDSCs, vector and mHIF-1α groups after implantation in nude mice for 30 and 60 days. The scale bar is 100 μm (n = 3). c Three-dimensional angiography images of blood vessels in two implanted scaffolds after implantation in nude mice for 30 and 60 days. The scale bar is 100 μm (n = 3). d, e Expression of VEGF, SDF-1 and PDGF at the protein level via WB detection in the scaffold tissue after 60 days (n = 3). (Unpaired, two-tailed t-test. In e-VEGF, **p = 0.0093, mHIF-1α+Heparin-free vs Control *p = 0.0249, Vector+Heparin-free vs Control *p = 0.0434; in e-PDGF, *p = 0.0003, p = 0.0079, *p = 0.016; in e, SDF-1, mHIF-1α+Heparin vs Control *p = 0.0006, mHIF-1α + Heparin-free vs Control *p = 0.0006, *p = 0.0249). f Comparative gene expression analysis of VEGF, PDGF and SDF-1 via qRT-PCR assay in the implanted scaffold tissue after 60 days (n = 3). (Unpaired, two-tailed t-test. In f, VEGF, **p = 0.0045, *p = 0.0104; in f, PDGF, p = 0.0025, *p = 0.0003; in f, SDF-1, mHIF-1α + Heparin vs Control p = 0.0025, mHIF-1α + Heparinfree vs Control p = 0.0069). Data are displayed as mean ± SD. (*p < 0.05, p < 0.01, *p < 0.001).
“Consequently, the ICP/MAP values of corpora cavernosa repaired by HIF-1α-mutated MDSCs-loaded scaffolds become comparable to those of normal corpora cavernosa and the relative maximum contraction force (MCF) is up to 77% of native corpora cavernosa,” concluded the researchers. “Besides, the newborn rabbits from the male rabbits treated by HIF-1α-mutated MDSCs-loaded scaffolds further confirm the recovery of physiological functions, including erectile function and ejaculation function, in the treated rabbits.”

Detection of intracavernosal pressures (ICP) and mean arterial pressure (MAP) and organ bath testing in the repaired cavernosa. a The diagram of measurement method of ICP and MAP. b, c After 6 V of electrical stimulation was applied to the cavernous nerve, the ICP/MAP value was recorded in six different groups after 2 (b) and 4 (c) months of implantation (n = 3). Data are displayed as mean ± SD and analysed by two-way ANOVA with Sidak’s multiple comparisons test in b (mHIF-1α vs Negative control: *P = 0.0482; positive control vs mHIF-1α: *P = 0.0215) and c (*P = 0.0276; NS, p > 0.05). d Images and schematic diagram showing organ bath testing of contraction force of repaired cavernosa at 37 °C, 95% oxygen and 5% carbon dioxide. The cavernous tissue (in the red dashed circles) was incubated in the Krebs solution and its contraction force was measured by a tension sensor under the constant oxygen flow. e Oscillogram of tension change by phenylephrine (green area) and phentolamine (blue area) stimulation of the repaired corpus cavernosum in each group (negative control, cell-free, MDSCs, vector and mHIF-1α or positive control group) after 4 months of implantation (n = 3). f Relative maximum contraction force (MCF) in five implantation groups (negative control, cell-free, MDSCs, vector and mHIF-1α groups) compared with that in the positive control group (mean MCF is defined as 1) after 4 months of implantation (n = 3). (Sidak’s multiple comparisons test, two-way ANOVA, *p = 0.0004; **p < 0.0001). Data are displayed as mean ± SD and analysed by GraphPad Prism software.
Regulatory Considerations and Safety

The birth time points and the numbers of newborn rabbits after different treatments in the five different groups. See also: Best 3D Printer Upgrades That Actually Improve Pri…. a Timeline of the experimental steps in the mating assessment. The arrows indicate the birth time points of newborn rabbits in the vector group (blue arrows) and the mHIF-1α group (red arrows). CC, corpus cavernosa. b The baby rabbits were born in one cage of the mHIF-1α group within after 2 months of the mating assessment. c The numbers of newborn rabbits in each group within 4 months of the mating assessment test (n = 5).
“Our work represents a significant step towards developing bioengineered vascularized corpora. It is the first report on 3D printed bioengineered scaffolds to successfully repair the defects and restore the erectile and ejaculation function, allowing the rabbits to recover their reproductive capability. Our strategy to repair cavernous tissue has outstanding value in accelerating the reconstruction of sinusoid structures. In addition to repairing the cavernosum tissue defects, these 3D-printed scaffolds have the potential to repair other vascularized tissues, such as skin, nasal tissue and myocardial tissue.”
While 3D printing scaffolds to assist in treatment of ED is more unique in terms of typical research connected with such technology, scientists around the world continue to perform a variety of studies involving neural scaffolds for spinal cord regeneration, titanium scaffolds imitating trabecular structures, and designs for bone tissue engineering.
Research Breakthroughs and Innovations
What do you think of this news? Let us know your thoughts; join the discussion of this and other 3D printing topics at 3DPrintBoard.com.
[Source / Images: ‘Functional reconstruction of injured corpus cavernosa using 3D-printed hydrogel scaffolds seeded with HIF-1α-expressing stem cells’]
The post Bioprinting Yields Promising Results for Treatment of Erectile Dysfunction appeared first on 3DPrint.com | The Voice of 3D Printing / Additive Manufacturing.
from Your daily news from 3DPrint.com https://bit.ly/3dZn7Wh
Frequently Asked Questions
How is 3D printing used in medicine?
3D printing is used in medicine for surgical planning models, custom implants, bioprinting tissue scaffolds, drug delivery systems, dental aligners, and prosthetics. It enables patient-specific solutions that improve outcomes and reduce surgery time.
What materials are biocompatible for 3D printing?
Common biocompatible materials include PEEK, titanium alloys (Ti6Al4V), bio-ceramics (hydroxyapatite), medical-grade resins, PLA for temporary implants, and hydrogels for bioprinting. Material choice depends on the application and required mechanical properties.
Is 3D printed medical equipment FDA approved?
Yes, several 3D printed medical devices have FDA clearance, including orthopedic implants, dental restorations, and surgical guides. Each device must go through the appropriate regulatory pathway based on its risk classification.
📌 Related Articles
- Best Budget 3D Printer Upgrades That Actually Improve Print Quality: Belts, Springs, Hotends & More
- Best 3D Printer Upgrades That Actually Improve Print Quality: Complete 2026 Guide
- Prusa Research Mini+ vs Prusa MK4: Full Specs Comparison & Buyer’s Guide
- ABS 3D Printing Settings Guide: Temperature, Enclosure, and Cooling for Strong Parts
- Bambu Lab P1S vs Bambu Lab P2S: Full Specs Comparison & Buyer’s Guide