Quick Answer: 3D Printed Boluses vs. Traditional Wax
Bottom Line: 3D printed nose boluses outperform traditional wax boluses in accuracy, cost-effectiveness, and reproducibility. When printed with 100% shell infill density and filled with water, they accurately replicate reference plan dosimetry while requiring less technical skill and reducing material costs by approximately 50%.
Key Findings:
- Volume Accuracy: 100% 3D printed shells showed only 1.31 ± 2.63 cm³ difference from virtual bolus, compared to -3.05 ± 11.06 cm³ for wax
- Cost Savings: 3D printed boluses cost significantly less in materials and staff time
- Print Time: 18% infill shells: 529 minutes | 100% infill shells: 747 minutes
- Reproducibility: 3D printed shells offer consistent results regardless of technician skill level
Comparison: 3D Printed Bolus vs. Traditional Wax Bolus
| Factor | Wax Bolus | 3D Printed Bolus |
|---|---|---|
| Volume Accuracy | -3.05 ± 11.06 cm³ difference | 1.31 ± 2.63 cm³ difference |
| Material Cost | Higher (wax, tools, water bath) | Lower (PLA filament) |
| Staff Time | Higher (labor-intensive process) | Lower (automated printing) |
| Technical Skill Required | High (manual craftsmanship) | Low (automated process) |
| Reproducibility | Variable (depends on technician) | High (consistent digital printing) |
| Skin Contact Quality | Variable (air cavity flaws possible) | Superior (precise patient surface contact) |
Comparison: 3D Printing Infill Options
| Parameter | 18% Infill Shell + Water | 100% Infill Shell + Water | 100% Infill Shell + Wax |
|---|---|---|---|
| Volume Difference | -1.03 ± 8.09 cm³ | 1.31 ± 2.63 cm³ | Similar to 100% water |
| Dosimetric Accuracy | Lower accuracy | Highest accuracy (P > 0.05) | High accuracy |
| Print Time | 529 minutes | 747 minutes | 747 minutes |
| Intraclass Coefficient | 0.48-0.88 | 0.48-0.88 (water fill) | 0.69-0.96 |
| Recommended Use | Less accurate option | Best for dosimetry | Alternative to water |
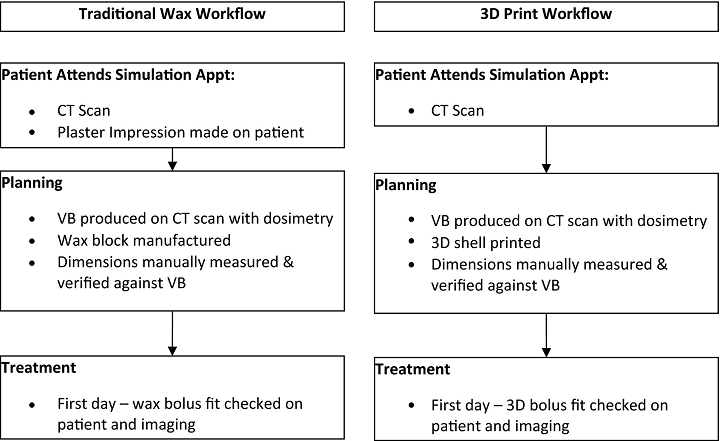
Boluses are used often to protect the body from radiotherapy targeted at specific areas, and 3D printing can help streamline their production. Four Australian researchers published a paper, titled “Comparison of 3D printed nose bolus to traditional wax bolus for cost-effectiveness, volumetric accuracy and dosimetric effect”, about their work evaluating the dosimetric and volumetric, and cost, differences between a 3D printed nose bolus and one made with traditional wax.
“Three-dimensional printing allows the conversion of digital models from data sets created via 3D ultrasound, computed tomography (CT) and magnetic resonance imaging into physical objects,” the team wrote. “In radiotherapy, 3D printed bolus is gaining momentum as the ideal patient bolus due to its durability, and superior patient surface contact over manually manufactured wax or gel bolus.”
Why Nose Boluses Are Challenging
Because of its contour changes, the nose is one of the most difficult areas to treat when it comes to skin cancer. But, to ensure that a full dose of radiotherapy is delivered to the patient’s skin surface, along with a homogenous dose distribution to the nose, it’s important that the bolus covers and conforms to the nose.
A radiotherapy bolus is a tissue-equivalent material placed on the skin surface to modify the dose distribution of radiation beams. It helps ensure that superficial tissues receive the prescribed dose, particularly in areas like the nose where the contour changes can create dose irregularities. Traditional bolus materials include wax, gel, and various plastics, each with their own limitations in terms of fit, reproducibility, and dosimetric accuracy.

Bolus Construction: (a) Creating a plaster impression, (b) plaster impression, (c) 3D printed nose bolus without fill (green) and wax bolus (red), (d) 3D shell with varied internal fill, 18% print fill and 100% print fill and (e) Nose bolus: wax (grey), 3D print and water fill (blue), 3D print and wax fill (red).
The Wax Bolus Process
It’s a labor intensive process to make a nose bolus out of wax, as the technician’s skill level can affect the dosimetric and volumetric accuracy, and there can also be variations from the process itself, like imperfect skin contact or air cavity flaws. But a 3D printed bolus doesn’t have these issues.
The traditional wax bolus fabrication process involves several manual steps that introduce variability. First, a plaster impression is taken of the patient’s nose using alginate material. This impression is then filled with Plaster of Paris to create a positive model. The technician then manually applies wax to this model, shaping it to achieve the desired thickness and contour. This process requires significant skill and experience to achieve consistent results. Variations in technique can lead to differences in bolus thickness, surface conformity, and ultimately, dosimetric accuracy.
“This study aimed to examine the volume, dimensional and dose differences between manually manufactured wax bolus and a 3D printed shell to the virtual bolus demonstrated in a radiotherapy plan for photon treatment to the nose, and to explore which type of bolus is more cost-effective to produce,” the researchers explained.
Study Methodology
The team enlisted 24 volunteers, and took plaster impressions of their noses using alginate and Plaster of Paris. Each positive plaster impression was CT scanned in 2 mm slices, and the scans were imported into the treatment planning system (TPS), contoured, and then “3D planned with virtual bolus and parallel opposed 6 MV lateral fields with collapsed cone algorithm.” Each virtual bolus (VB) plan was manufactured the traditional way, using wax, and then 3D printed out of PLA on an Ultimaker 2+.
3D Printing Parameters
A duplicate was fabricated for each 3D printed shell in order to check for conformity of fit and reproducibility. The 3D printing parameters included:
- 0.2 mm layer height
- 0.5 mm external perimeter thickness
- 0.8 mm top/bottom thickness
- 100% and 18% fill density
“To compare volume variations and dosimetry, each constructed bolus was CT scanned and a plan replicating the reference plan fields generated,” the researchers wrote.
Dosimetric Analysis
Each bolus was contoured, and then assessed via CT scanning for any volume variations from the “reference plan’s VB contours.” Then, the plaster impression plans were copied to the CT image data set for the two types of bolus, and the team recorded and compared the dose at four different points.
“Points A, B and C were placed as close as possible to the same position across plans, accepting differences in exact point position (real slice or between slices) and that the bolus was not perfectly straight on each scan,” the researchers explained. See also: Best 3D Printer Upgrades That Actually Improve Pri…. “Additionally, a pseudo-PTV was created on the VB plan, copied to all other bolus data sets, and maximum and mean doses to this volume recorded.”
Volume and Dimensional Analysis
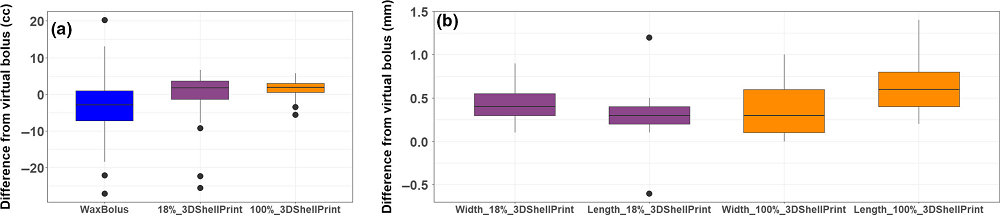
Data analysis. (a) Volume difference of wax, 18% shell 3D print and 100% shell 3D print to the virtual bolus, (b) dimensional difference of wax, 18% shell 3D print and 100% shell 3D print to the virtual bolus.
They also computed dose calculations for more dosimetric analysis – once on the 18% infill shells with water fill, and twice on the 100% shells, with water fill and then with wax fill. CT scans were performed, and the team calculated the difference in dose distribution for each defined point, and the maxium and mean doses to the pseudo-PTV for both the original reference plan and the boluses.
Visual Assessment Results
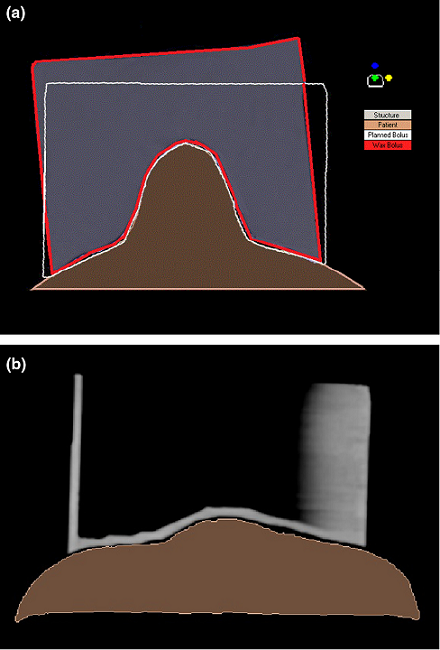
Nose bolus. (a) Difference between planned (white outline) and manufactured wax nose bolus (red outline) and (b) demonstration of an indistinct bolus edge.
The researchers wrote, “Mean volume differences between the virtual bolus (VB) and wax, and the VB and 18% and 100% 3D shells were -3.05 ± 11.06 cm³, -1.03 ± 8.09 cm³ and 1.31 ± 2.63 cm³, respectively. While there was no significant difference for the point and mean doses between the 100% 3D shell filled with water and the VB plans (P> 0.05), the intraclass coefficients for these dose metrics for the 100% 3D shell filled with wax compared to VB doses (0.69-0.96) were higher than those for the 18% and 100% 3D shell filled with water and the wax (0.48-0.88).”
Dose Point Analysis

Dose point difference from reference plan. The outliers can be attributed to the same scans. The 18% shell outliers all belong to the same single subject’s plan as generated on the CT scan of their physical 18% shell nose bolus, and the outliers on the 100% shells are all from the same three volunteers plan generated on the CT scan of their physical 100% shell nose bolus.
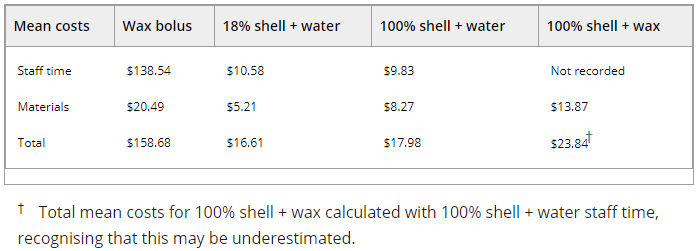
Cost Analysis
The manufacturing time, and material costs, of fabricating the boluses were also analyzed. The team focused on consumable costs for this, and did not include the 3D printer’s purchase cost, maintenance and future replacement of its parts, and the tools and water bath for the wax bolus. Three of the 48 3D printed boluses did not completely print, and time lost on these was also left out of the cost analysis.
You can see in the table below that average costs for materials and staff time were higher for the wax boluses than for the 3D printed ones. Average time to 3D print the 18% infill shells was 529 minutes, while it took 747 minutes to print the 100% infill shells.
“As the 18% shells were converted and completed prior to all the 100% shells, the total cost of staff time is higher for the 18% shell group due to staff being more familiar with the process of DICOM to .stl file conversion for the 100% shell group,” the researchers explained.
Study Limitations
It’s important to note several limitations of this study. The cost analysis only considered consumable materials and staff time, excluding capital equipment costs such as the 3D printer purchase price, maintenance, and replacement parts. Similarly, costs for wax bolus tools and water baths were not included. Additionally, three of the 48 3D printed boluses did not print completely, and the time lost on these failed prints was excluded from the cost analysis, potentially skewing the results slightly in favor of 3D printing.
The study also focused specifically on nose boluses for photon radiotherapy, so the results may not directly apply to other anatomical sites or different radiation modalities such as electron therapy. Further research would be valuable to validate these findings across different treatment sites and radiation types.
Conclusions and Clinical Impact
Overall, the 3D printed boluses for photon nose treatments were more accurate and cost-effective than their wax counterparts, and will likely result in a better experience for patients.
“When printed in 100% shell infill density, and filled with water, 3D bolus shells accurately replicate the reference plan dosimetry. Three-dimensional printed bolus shells produce superior bolus geometry, are more cost-effective to produce than traditional wax bolus and do not require the same technical skills for production as traditional wax bolus,” the researchers concluded.
The findings from this study have significant implications for radiotherapy departments looking to improve their bolus fabrication processes. By adopting 3D printing, departments can reduce costs while improving the accuracy and reproducibility of their boluses. This is particularly important for challenging anatomical sites like the nose where achieving precise dose distributions is critical for treatment success.
Furthermore, the reduced dependence on technician skill level means that 3D printing can help standardize bolus production across different staff members and even different treatment centers. See also: Best Budget 3D Printer Upgrades That Actually Impr…. This standardization could lead to more consistent patient outcomes and easier training for new staff.
Future Directions
The success of 3D printed boluses in this study opens up several avenues for future research and clinical implementation. One area of interest is the exploration of different 3D printing materials beyond PLA, including flexible and radiographically equivalent materials that may offer additional advantages in terms of patient comfort and dosimetric accuracy.
Another promising direction is the integration of 3D printed boluses directly into the treatment planning workflow, potentially enabling on-demand bolus fabrication that can be optimized for each individual patient’s anatomy and treatment plan. This could further reduce wait times and improve the personalization of radiotherapy treatments.
As 3D printing technology continues to advance, we can expect to see faster print times, lower costs, and improved material properties, all of which will contribute to making 3D printed boluses an increasingly attractive option for radiotherapy departments worldwide.
Frequently Asked Questions
1. What is a radiotherapy bolus and why is it needed?
A radiotherapy bolus is a tissue-equivalent material placed on a patient’s skin surface to modify the radiation dose distribution. It’s particularly important for treating superficial tumors, as it helps ensure that the skin surface receives the prescribed dose. Without a bolus, high-energy radiation beams can deposit insufficient dose at the skin surface, potentially undertreating superficial cancer cells. The bolus acts as a “buildup” material, allowing the radiation dose to reach maximum at the skin surface rather than deeper in the tissue.
2. How accurate are 3D printed boluses compared to traditional wax boluses?
According to the Australian study, 3D printed boluses demonstrated significantly better volumetric accuracy than wax boluses. The mean volume difference from the virtual bolus was only 1.31 ± 2.63 cm³ for 100% infill 3D printed shells, compared to -3.05 ± 11.06 cm³ for wax boluses. This represents a substantial improvement in consistency and precision. Additionally, when printed with 100% shell infill and filled with water, the 3D printed boluses accurately replicated reference plan dosimetry with no statistically significant difference (P > 0.05).
3. What are the cost differences between 3D printing and wax bolus fabrication?
The study found that 3D printed boluses were more cost-effective than wax boluses when considering both material costs and staff time. While the exact monetary savings depend on local pricing and labor costs, the research clearly showed that the combination of lower material costs (PLA filament vs. wax and associated materials) and reduced staff time made 3D printing the more economical option. It’s worth noting that the cost analysis excluded capital equipment costs like the 3D printer purchase price, so the long-term economic benefits become even more apparent as the initial investment is amortized over multiple patients.
4. How long does it take to 3D print a nose bolus?
Based on the study parameters, printing a nose bolus on an Ultimaker 2+ with 0.2 mm layer height took approximately 529 minutes (about 8.8 hours) for 18% infill shells and 747 minutes (about 12.5 hours) for 100% infill shells. These print times are for shells only, which are then filled with either water or wax. While this may seem lengthy, it’s important to consider that the printing process is largely automated, requiring minimal staff intervention compared to the labor-intensive manual wax bolus fabrication process. Advances in 3D printing technology, including faster printers and optimized slicing parameters, could potentially reduce these times in the future.
5. What 3D printing parameters were used in the study?
The researchers used an Ultimaker 2+ 3D printer with PLA material and specific parameters optimized for radiotherapy bolus production. The key settings included 0.2 mm layer height, 0.5 mm external perimeter thickness, 0.8 mm top/bottom thickness, and either 18% or 100% fill density. These parameters were chosen to balance structural integrity with printing efficiency and dosimetric accuracy. The 100% infill shells with water fill proved to be the most accurate for dosimetric purposes, though the 18% infill shells offered faster print times for situations where slightly reduced accuracy is acceptable.
6. Do 3D printed boluses require special technical skills to produce?
One of the significant advantages of 3D printed boluses is that they require less technical skill to produce compared to traditional wax boluses. While some training is needed for DICOM to STL file conversion and 3D printer operation, the process is largely automated and standardized. This reduces the dependence on highly skilled technicians and makes it easier to train new staff. In contrast, wax bolus fabrication requires considerable manual dexterity and experience to achieve consistent results, with significant variation possible based on the individual technician’s skill level.
7. Can 3D printed boluses be used for other body parts besides the nose?
While this study focused specifically on nose boluses for photon radiotherapy, the principles and findings likely extend to other anatomical sites as well. The 3D printing approach could be particularly valuable for other complex anatomical contours where achieving precise bolus fit is challenging, such as the ear, fingers, or toes. However, additional research would be valuable to validate the accuracy and cost-effectiveness of 3D printed boluses for these different sites. The methodology of creating patient-specific boluses from CT or MRI scans is broadly applicable across the body.
8. What are the limitations of the study?
The study had several important limitations to consider. First, the cost analysis excluded capital equipment costs (3D printer purchase, maintenance, and replacement parts) as well as wax bolus tool costs, which could affect the economic conclusions in different settings. Second, three of 48 3D printed boluses failed to print completely, and the time lost on these failures was excluded from the cost analysis. Third, the study focused specifically on photon radiotherapy for the nose, so results may not directly apply to other radiation modalities or anatomical sites. Finally, the relatively small sample size of 24 volunteers means that larger studies would be beneficial to confirm these findings.
9. What materials were used for the 3D printed boluses?
The study used PLA (polylactic acid) filament as the printing material for the 3D printed bolus shells. PLA is a common biodegradable thermoplastic derived from renewable resources like corn starch or sugarcane. It’s widely available, relatively inexpensive, and prints well on most desktop 3D printers. The hollow shells were then filled with either water or wax to achieve the desired density for radiotherapy purposes. While PLA was effective in this study, future research may explore alternative 3D printing materials that offer additional benefits such as improved flexibility, better radiographic equivalence, or enhanced durability.
10. How does 3D printing improve patient experience in radiotherapy?
3D printed boluses can improve patient experience in several ways. First, the superior surface contact and fit of 3D printed boluses can make them more comfortable for patients to wear during treatment, compared to wax boluses which may have irregularities or air gaps. Second, the improved accuracy and consistency of 3D printed boluses may lead to better treatment outcomes, which is ultimately the most important factor for patient satisfaction. Third, the faster production workflow enabled by 3D printing could potentially reduce wait times for patients needing bolus fabrication. Finally, knowing that their treatment is being supported by cutting-edge technology may provide patients with increased confidence in their care.
Sources and References
- “Comparison of 3D printed nose bolus to traditional wax bolus for cost-effectiveness, volumetric accuracy and dosimetric effect” – Journal of Medical Radiation Sciences
- Custom 3D Printed Boluses – 3DPrint.com
- Treating Cancer Patients Using 3D Scanning & Printing to Create the Bolus – 3DPrint.com
Discuss this and other 3D printing topics at 3DPrintBoard.com or share your thoughts below.
Related: Rice University Researchers Develop a New 4D Printing Method to Create Shapeshif · Researchers Introduce New LITA Method of Carbon Fiber 3D Printing · Australian Researchers 3D Printing Tactile Sensors with TPU and PLA Composites
📌 Related Articles
- Best 3D Printer Upgrades That Actually Improve Print Quality: Complete 2026 Guide
- Best Budget 3D Printer Upgrades That Actually Improve Print Quality: Belts, Springs, Hotends & More
- ABS 3D Printing Settings Guide: Temperature, Enclosure, and Cooling for Strong Parts
- Prusa Research Mini+ vs Prusa MK4: Full Specs Comparison & Buyer’s Guide
- 3D Printing Safety Equipment Guide: Respirators, Gloves, and Ventilation for 2026