Swiss researchers are investigating how 3D printed mandibular models can help offer improved, patient-specific treatment by investigating the best technology possible. Detailing their findings in ‘Evaluation of the Dimensional Accuracy of 3D-Printed Anatomical Mandibular Models Using FFF, SLA, SLS, MJ, and BJ Printing Technology,’ we learn how a variety of different techniques may benefit both medical professionals and patients.
As 3D printing continues to infiltrate a wide range of industries—and medical applications too—many different methods and materials are available to create 3D printed models that assist in the diagnosis of health conditions, treatment, education, and surgery. Models and implants are being 3D printed more often today with good success, helping patients recover and enjoy a better quality of life after surgery to remove tumors in the jaw area; however, challenges still exist in creating fully functional anatomical models without a variety of inaccuracies and deformations.
The Role of 3D Printing in Medicine
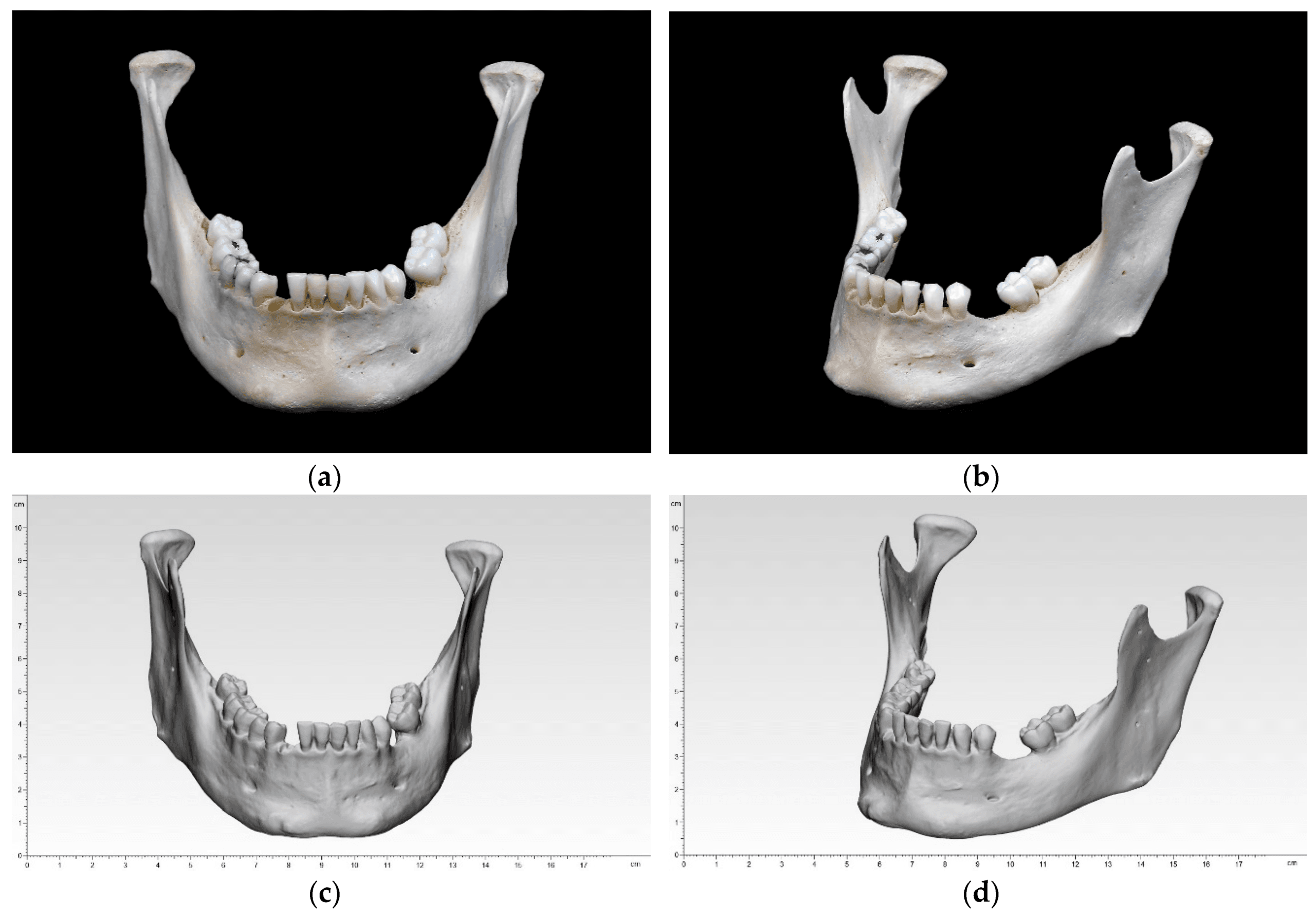
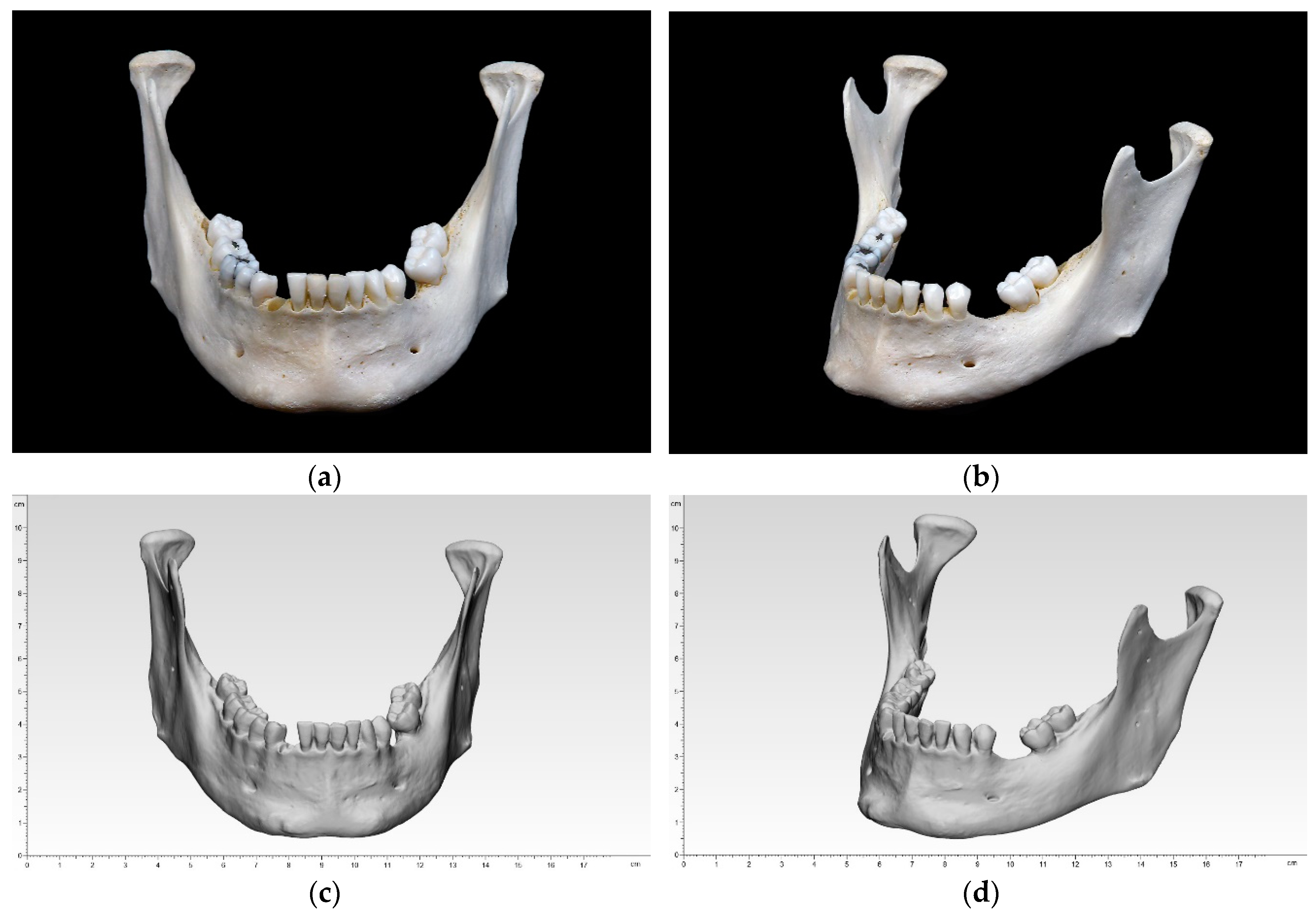
Bony mandibular reference: (a) front view; (b) side view; digitized mandibular (standard tessellation file (STL)) in 3-matic medical: (c) front view; (d) side view.
During this study, the researchers skipped straight to creating the .stl file on a high-precision scanner, noting that their process resulted in ‘significant reduction of error sources.’ Their overall goal was to compare 3D printed mandibular models created through different techniques. Ten different samples of a dry human bony mandible were fabricated on five different types of 3D printing technology.
Biocompatible Materials and Processes
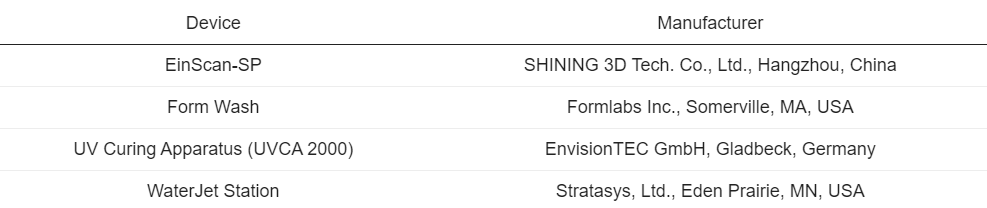
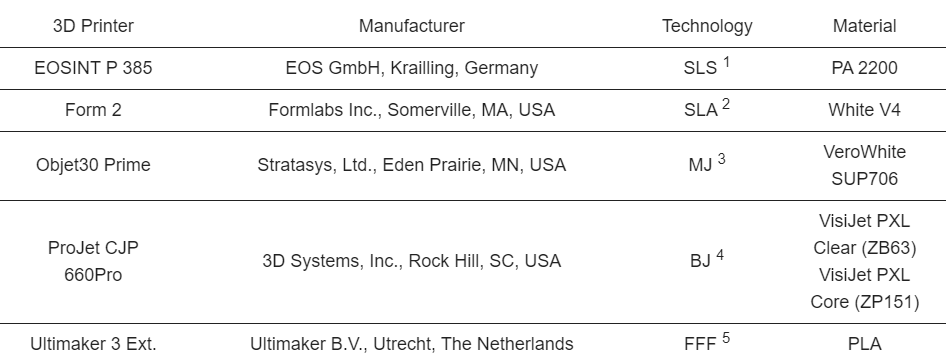
Three-dimensional (3D) printers, manufacturers, technology, and material
“To leave the occlusal plane untouched for later analysis and to minimize the number of support structures required, all models were aligned vertically,” explained the researchers.
Clinical Applications and Case Studies
“Minor adjustments were made in the 3D slicer software before 3D printing. These adjustments ensured that the printing conditions corresponded to a clinical routine with a reasonable printing time and printing costs for a single model. According to the applied 3D printing technology, an adequate post-processing was conducted.”
Results regarding each method of technology were as follows:
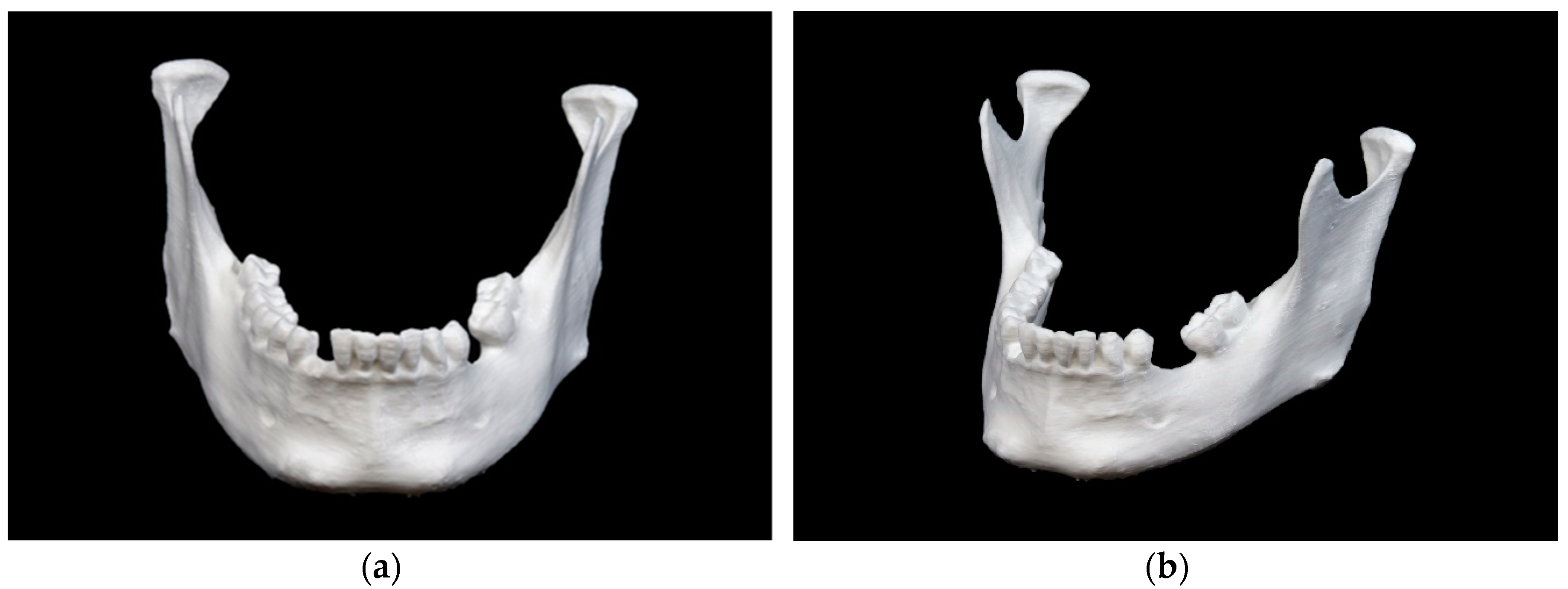
- FFF 3D printing – Small pieces of support structures were noted, and ramus region markings were ‘quite blurred.’
- SLA technology – surfaces were smooth, although interdental space was ‘not adequately shaped.’ Ramus region markings were noted as well-defined.
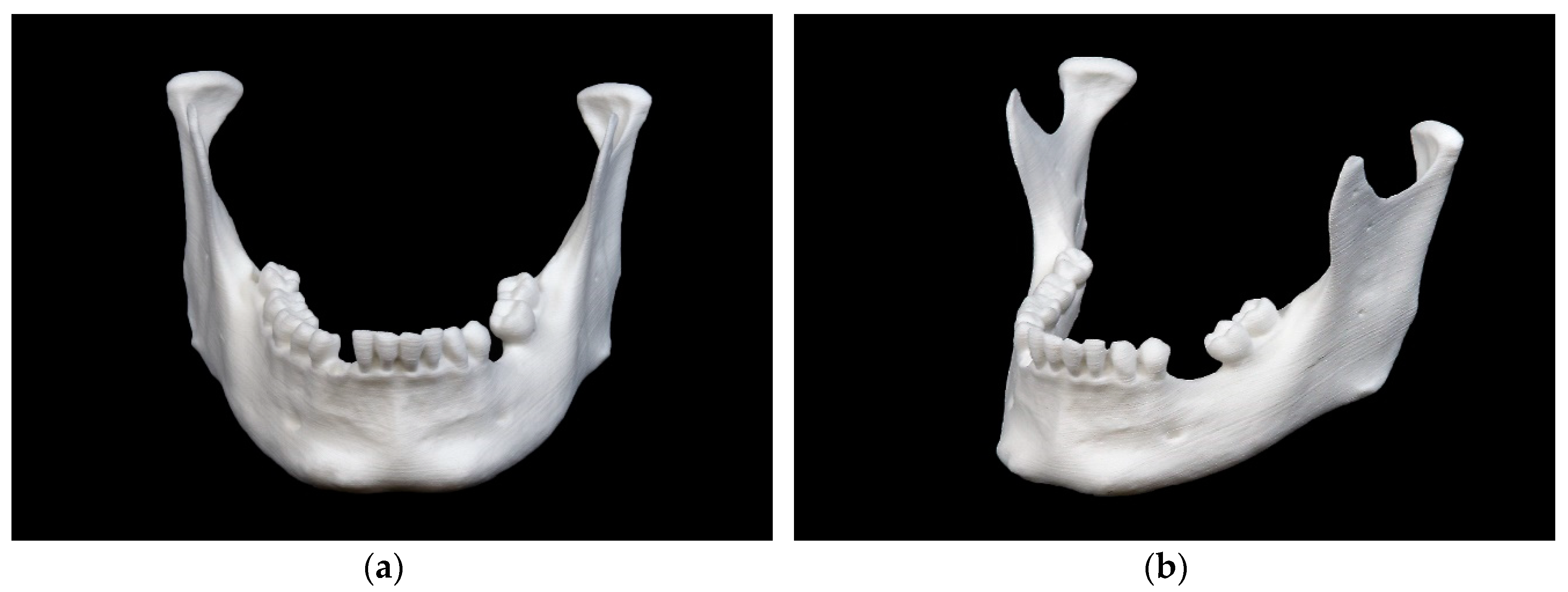
- SLS technology – ‘subtly recognizable layer lines’ were displayed, and the ramus region exhibited clear markings.
- Material-jetting 3D printing – Produced glossy and matte surfaces, but ramus region markings were ‘clearly visible’ no matter what.
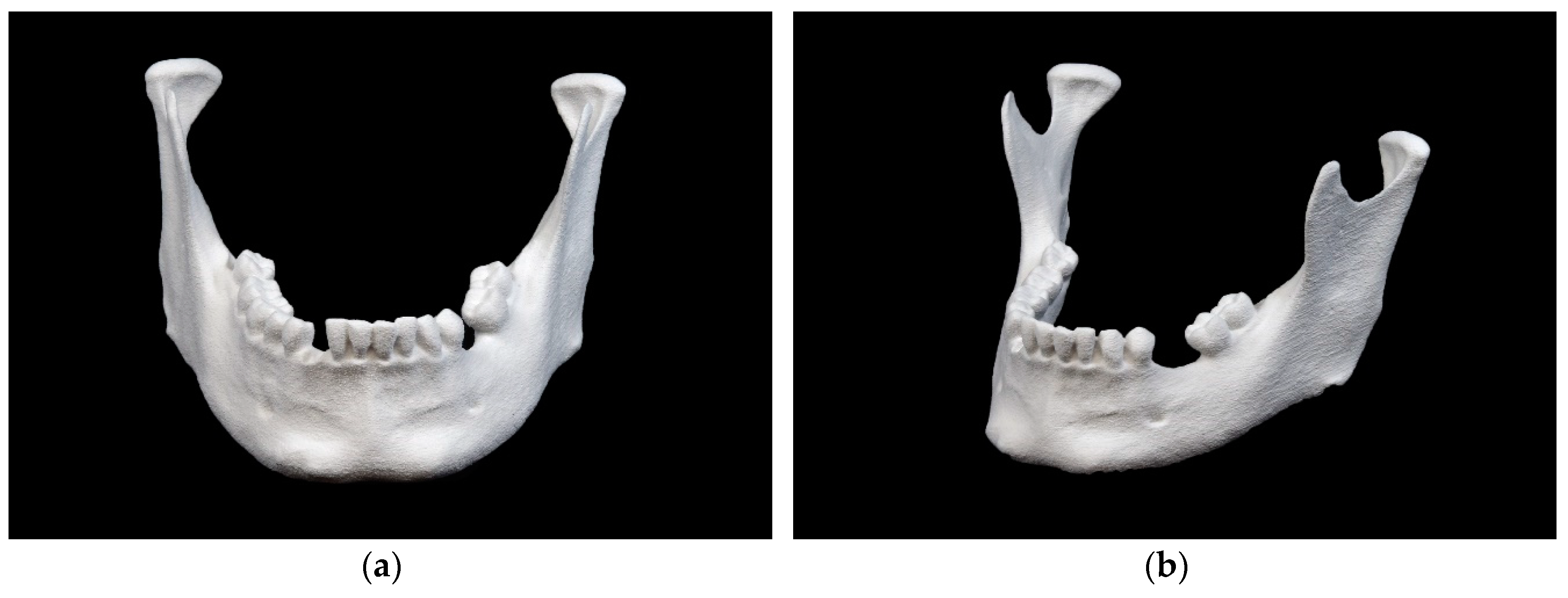
- Binder-jet 3D printing – Resulted in a porous surface. Ramus region markings were ‘not very clear’ because of the rough surface.
Regulatory Considerations and Safety
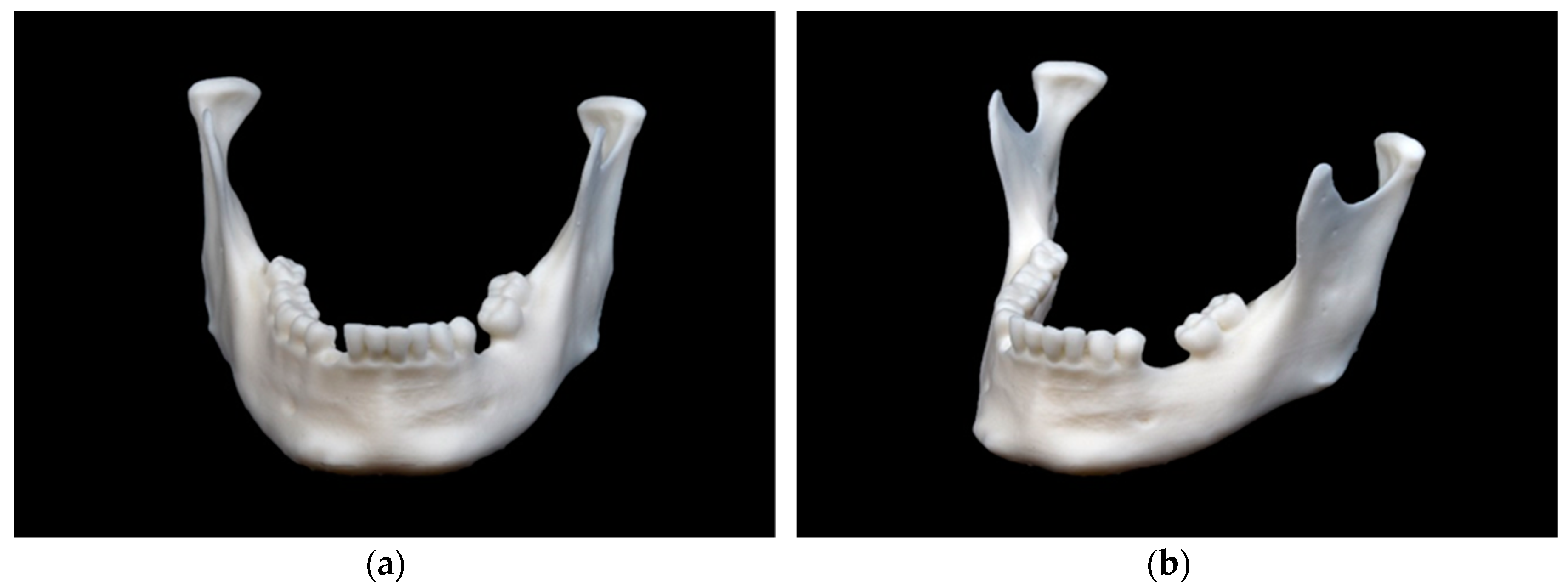
Mandibular model printed in fused filament fabrication (FFF) technology: (a) front view; (b) side view.
Research Breakthroughs and Innovations
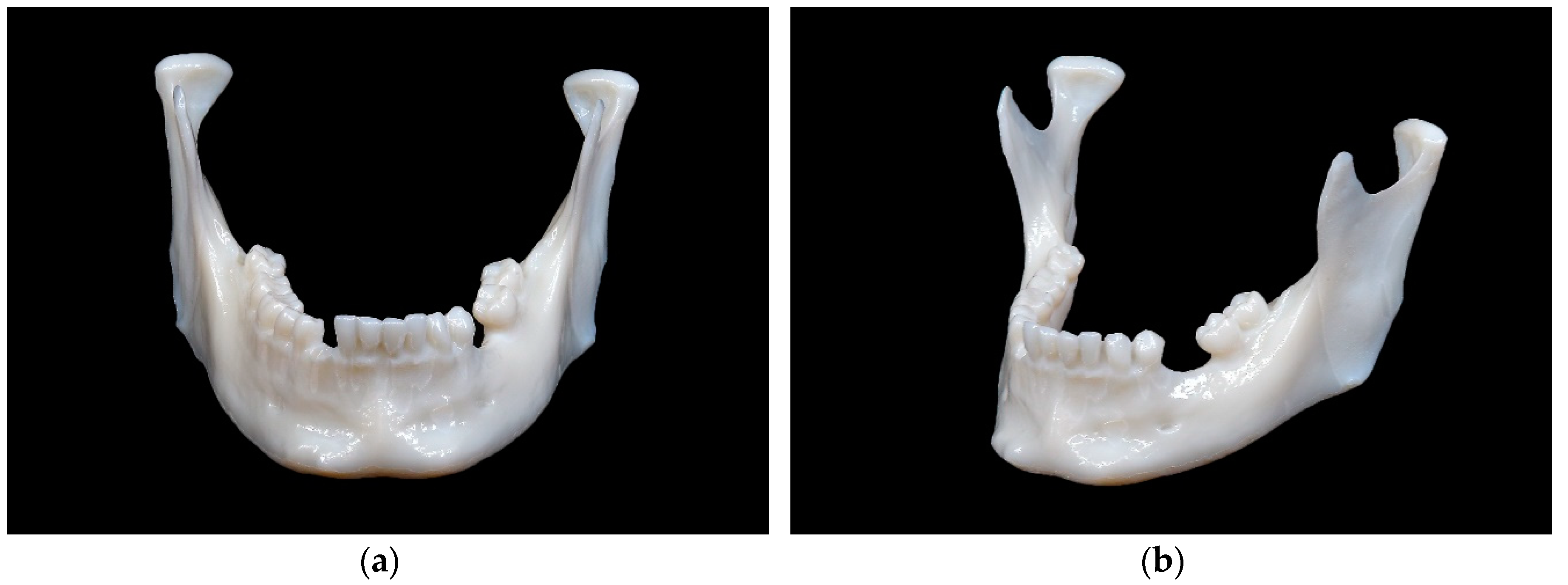
Mandibular model printed in selective laser sintering (SLS) technology: (a) front view; (b) side view.
The Future of Bioprinting and Medical AM
Mandibular model printed in binder jetting (BJ) technology: (a) front view; (b) side view.
“The findings here showed that all of the five evaluated printing technologies are very accurate. The SLS printer has the highest overall trueness (RMS 0.11 ± 0.016 mm), whereas the FFF printer has the highest overall precision (RMS 0.05 ± 0.005 mm). Despite the existing statistical significance of the differences in accuracy between all the 3D printers studied, when regarded separately, all are minor and acceptable for medical–surgical applications,” concluded the researchers.
“A broad range of cost-effective in-house desktop 3D printers based on simple AM technologies, e.g., FFF technology, offer both high accuracy and the ability to process a wide range of different printing materials, including a growing number of biocompatible materials. This qualifies them for most medical–surgical applications, such as the fabrication of anatomical models for the pre-bending of osteosynthesis plates, for surgical drilling and cutting guides, for implants, or simply for educational purposes.”
What do you think of this news? Let us know your thoughts! Join the discussion of this and other 3D printing topics at 3DPrintBoard.com.
The Role of 3D Printing in Medicine
[Source / Images: ‘Evaluation of the Dimensional Accuracy of 3D-Printed Anatomical Mandibular Models Using FFF, SLA, SLS, MJ, and BJ Printing Technology’]
The post Comparison 3D Printing Techniques for Anatomical Mandibular Models appeared first on 3DPrint.com | The Voice of 3D Printing / Additive Manufacturing.
Related Articles
Frequently Asked Questions
How is 3D printing used in medicine?
3D printing is used in medicine for surgical planning models, custom implants, bioprinting tissue scaffolds, drug delivery systems, dental aligners, and prosthetics. It enables patient-specific solutions that improve outcomes and reduce surgery time.
What materials are biocompatible for 3D printing?
Common biocompatible materials include PEEK, titanium alloys (Ti6Al4V), bio-ceramics (hydroxyapatite), medical-grade resins, PLA for temporary implants, and hydrogels for bioprinting. Material choice depends on the application and required mechanical properties.
Is 3D printed medical equipment FDA approved?
Yes, several 3D printed medical devices have FDA clearance, including orthopedic implants, dental restorations, and surgical guides. Each device must go through the appropriate regulatory pathway based on its risk classification.
📌 Related Articles
- Best 3D Printer Upgrades That Actually Improve Print Quality: Complete 2026 Guide
- Best Budget 3D Printer Upgrades That Actually Improve Print Quality: Belts, Springs, Hotends & More
- Prusa Research Mini+ vs Prusa MK4: Full Specs Comparison & Buyer’s Guide
- Bambu Lab P1S vs Bambu Lab P2S: Full Specs Comparison & Buyer’s Guide
- Bambu Lab A1 vs Elegoo Centauri Carbon: Full Specs Comparison & Buyer’s Guide